Fighting Clinician Burnout
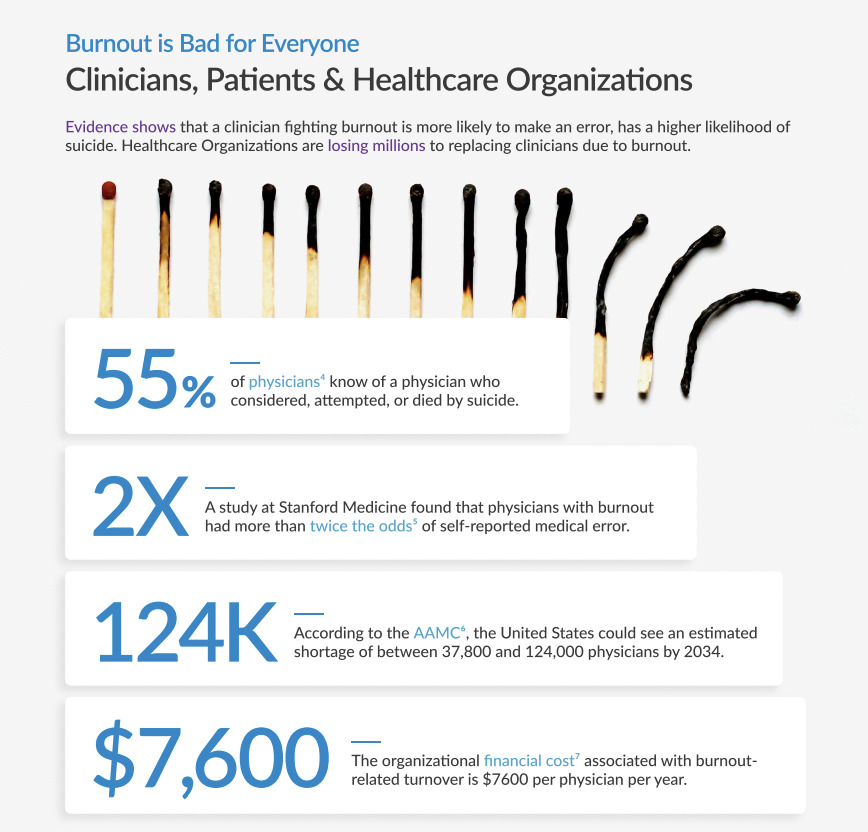
Clinician burnout is a crisis, not just a buzzword. At CareAlign we care about clinicians, so we created this page with information for clinicians and organizations on addressing burnout, both in the short and long term.
Interviews with Clinicians & Leaders
Strategies to Combat Burnout


4 Strategies to Retain Nurses
Clinician Mental Health in 2022
25X5 Symposium: Fighting Clinician Burnout
Solutions for Addressing Burnout
A key for all these solutions is that practicing clinicians should have a voice in decisions. Administrators should get feedback and ideas from all different clinicians prior to implementing solutions. Clinicians voice is key here!
Give Clinicians Agency
Many clinicians feel like they have no autonomy in their practice. They often do not get a say in appointment lengths, number of appointments each day, the flexibility of their schedule, the tools they use to do their work, and more. When clinicians see all the problems or inefficiencies throughout their day, there is often not much the clinician can do. Giving clinicians more autonomy – whether in their schedule, the tools they use, or other aspects of work – allows these clinicians to implement changes and feel more in control of their environment, which can help with burnout.
Have administrators shadow clinicians
Having administrators shadow or observe clinicians allows them to see clinicians workflow and understand why certain things are restrictive or problematic. The shadowing should be done for a long enough period of time for the leaders to see what a typical workday is like for the clinicians. Then, leaders and clinicians can work together to come up with solutions to problems. This observation or shadowing should be done consistently so that leaders can see how problems or solutions are evolving and best understand how to make new changes.
Reduce the administrative load, and consequently the time spent on work
Clinicians spend a lot of time on administrative work. A study of family medicine physicians found that physicians spend over 2.5 hours a day on documentation and administrative tasks. There are ways to reduce this administrative burden. First, using clinician-focused tech can save clinicians a lot of time on charting. Staffing support, such as using Medical Assistants and scribes, can reduce the workload for clinicians. Additionally, using team-based practices for things such as inbox management can allow physicians to focus on the tasks that most need their attention and allow other team members to apply their knowledge and skills and send just the things they cannot complete over to the physician. Finally, blocking a few patient appointment slots for administrative work allows clinicians to get the administrative work they do need to complete done at work, instead of bringing it home to do after hours.
Improve pay and benefits
Employees need to be compensated fairly for their work. Clinicians should get fair salaries with adequate raises. When clinicians realize they are being paid below what they are worth, then they will leave to find somewhere they will be more respected. Additionally, employers can provide benefits such as strong health insurance with mental health coverage, ample paid time off, paid sick leave, paid parental leave, retirement options, child care assistance, tuition reimbursement, money for transit (bus fares or gas compensation), and more. Learn what employees at the organization care about, and create benefits accordingly.
Reduce stigma and licensing concerns for clinicians seeking mental health treatment
Professional treatment can help clinicians struggling with burnout or mental health issues. However, not many seek this help. When asked why they don’t get professional help for mental health problems, almost half of physicians said they can deal with this without help from a professional, while over 40% said they don’t want to risk disclosure to a medical board. In 2018, the Federation of State Medical Boards (FSMB) recommended that licensing applications should be updated and should only ask about current issues that undermine a physician’s ability to work well; however, a 2020 study in JAMA found that only one state met all five FSMB licensure recommendations. Following the FSMB recommendations for licensure is important, as is the opportunity for clinicians to keep their mental health treatments private unless it could impact their ability to practice medicine or put others in harm’s way. In the long-term, organizations should work to reduce the stigma associated with mental health concerns. This is a difficult issue to tackle, but it is important in the long-term.
Improve workplace safety
Workplace safety is a big issue that impacts workers’ physical and psychological health. The American Nurses Association has found that one in four nurses are assaulted in the workplace, and only 20%-60% of incidents are reported. Additionally, a JAMA study found that almost a quarter of physicians experienced mistreatment in the past year, and that this mistreatment was associated with an increase in burnout and higher odds of intent to leave their job.
Creating and implementing a workplace violence prevention program can help improve safety. The plan should identify risks and implement strategies to mitigate them. The plan should include what to do if an issue occurs, and should have resources and guidelines for supporting clinicians after experiencing an issue. For this program to be successful, everyone needs to be trained on the program, and there needs to be anonymous online reporting for events so that people feel more comfortable speaking up when something goes wrong.
Sharp Conversations
Sharp Conversations is an interview series with real conversations about burnout with leaders in healthcare working to enact change. The series is co-hosted by Subha Airan-Javia, MD, FAMIA and Janae Sharp. Know someone in healthcare doing great work with burnout that you think should be interviewed? Email us at info@carealign.ai
Resources for Clinicians
The Emotional PPE Project
Connects healthcare workers in need with licensed mental health profes
Therapy Aid Coalition
Free short-term therapy for US essential workers
A nonprofit organization that empowers all physicians to provide high-quality care and take a leadership role in shaping the future of health care
Physician Support Line
A national, free, and confidential support line service made up of 600+ volunteer psychiatrists, joined together in the determined hope to provide peer support for physician colleagues and American medical students
PeerRxMed
A free, peer-supported program designed to help physicians and others on the care team move toward thriving both personally and professionally

